Despite the city state’s strict contact-tracing, quarantining and travel restrictions, a second wave of infections from returning residents and local transmissions saw cases spike from 100 to 1,000 in one month
Kok Xinghui
3 Apr, 2020
What a difference a month can make. At the beginning of March, Singapore had just over 100 coronavirus infections and countries across the world looked to the Southeast Asian city state for inspiration. Its aggressive contact tracing, strict quarantine procedures and measured travel restrictions received praise, as did its world-leading testing rates (as of March 25 it had carried out 6,800 tests per million people, more than other ‘leaders’ such as South Korea at 6,500 and Taiwan, at 1,000).
Indeed, if anything there may have been a touch of envy overseas at how this small but efficient country was managing to keep infections so low, even while keeping its schools and malls open and enjoying a semblance of normal life.
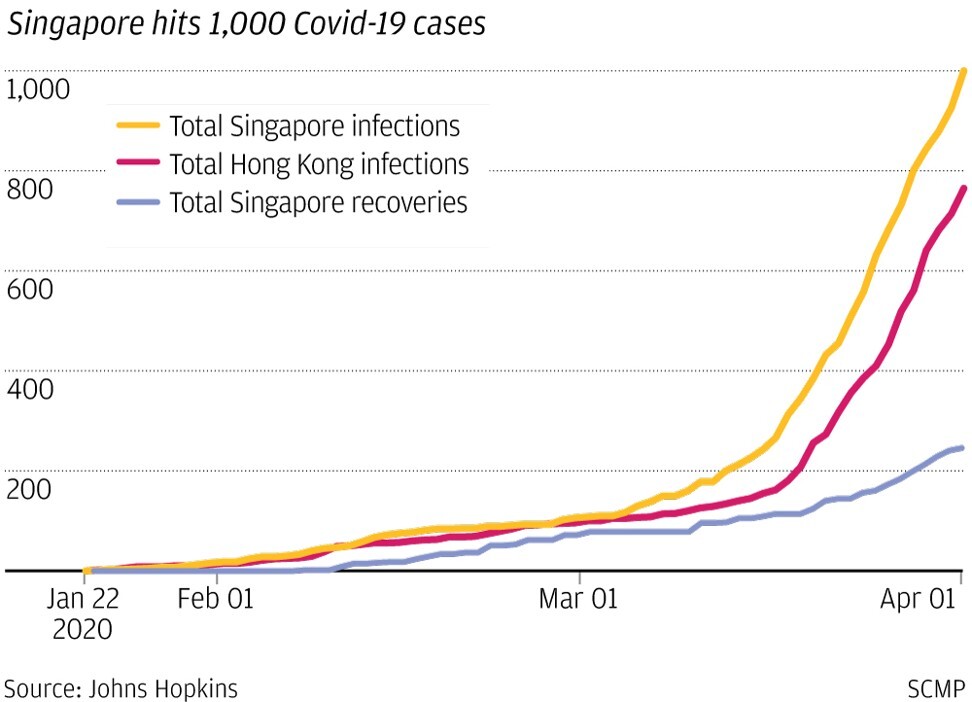
Fast forward to Wednesday, April 1, when Singapore passed the psychologically significant mark of 1,000 infections, and the picture wasn’t quite so rosy.
Throughout February, the number of new infections a day had stayed within single digits. On April 1 alone, there were 74 new cases. April 2 brought a further 49 infections and a fourth death, though 266 people in total had fully recovered from the illness.
How did this happen?
THE SECOND WAVE
Experts say the surge of cases in this country of 5.7 million people represents a “second wave” of infections.
The first wave began when tourists from mainland China passed the virus to Singapore residents in the initial stages of the global outbreak, with the earliest cases happening before the city state had implemented any travel restrictions.
As the number of cases grew, the city state introduced increasingly strict travel restrictions, first targeting foreign travellers coming from China, then Korea, Italy and Iran, and eventually barring all travellers.
However, a large part of the second wave of infections involves Singapore residents returning from countries such as the United States and Britain, which are experiencing a surge of cases.
Even more worryingly for authorities, the second wave also includes an increasing number of locally transmitted infections and cases with no known links to confirmed patients.
In response to the second wave, the city state introduced stricter social distancing measures, barring the entry of all travellers from March 23 and on March 27 closing bars and nightlife venues, limiting gatherings to 10 people and introducing penalties for individuals and restaurants who failed to keep customers one metre apart. Residents were urged to stay home and go out only to get essentials.
This week National Development minister Lawrence Wong, who co-chairs a coronavirus task force, said the next two weeks would be “critical” in demonstrating whether these measures were working.
He said the government needed to “get all Singaporeans to understand that every person is in fact on the front line”.
On February 29, there were just six local clusters of infections; by the beginning of April there were more than 20, among them a bridal studio, workers’ dormitories, and a nursing home with 11 cases, including a 102-year-old woman. Mustafa Centre, a popular shopping haunt for both residents and tourists in the Little India district, is linked to 11 infections.
“Definitely, all of us should be worried about the second wave,” said Associate Professor Jeremy Lim from the global health programme at the Saw Swee Hock School of Public Health.
WEAK LINK
Alarming as the rise in cases may seem, Singapore’s infection rate is not extraordinary in a global context. On February 29, there were 86,604 cases worldwide and this had grown almost tenfold to 858,361 by March 31. Hong Kong saw an increase from 95 to 715 in the same time period.
As Michael Osterholm, an infectious disease expert at the University of Minnesota, told Reuters: “Singapore’s approach has been by far one of the very best. What they are really showing the rest of the world is that this is just a difficult virus to beat back and keep down.”
Even so, given Singapore has taken what the World Health Organisation describes as a “leave no stone unturned” approach – though without yet having resorted to a lockdown – experts are concerned at why its containment strategy has not been more successful.

Kitty Lee, partner and head of Health and Life Science at the Asia-Pacific arm of consulting firm Oliver Wyman, described the situation as “a bit frightening”.
Lee said residents were “lax” when it came to social distancing, noting that only 40 per cent of employees in the central business district were working from home.
Singapore authorities have since warned employers that those who do not implement telecommuting while being able to do so will face prosecution.
He said the government needed to “get all Singaporeans to understand that every person is in fact on the front line”.
On February 29, there were just six local clusters of infections; by the beginning of April there were more than 20, among them a bridal studio, workers’ dormitories, and a nursing home with 11 cases, including a 102-year-old woman. Mustafa Centre, a popular shopping haunt for both residents and tourists in the Little India district, is linked to 11 infections.
“Definitely, all of us should be worried about the second wave,” said Associate Professor Jeremy Lim from the global health programme at the Saw Swee Hock School of Public Health.
WEAK LINK
Alarming as the rise in cases may seem, Singapore’s infection rate is not extraordinary in a global context. On February 29, there were 86,604 cases worldwide and this had grown almost tenfold to 858,361 by March 31. Hong Kong saw an increase from 95 to 715 in the same time period.
As Michael Osterholm, an infectious disease expert at the University of Minnesota, told Reuters: “Singapore’s approach has been by far one of the very best. What they are really showing the rest of the world is that this is just a difficult virus to beat back and keep down.”
Even so, given Singapore has taken what the World Health Organisation describes as a “leave no stone unturned” approach – though without yet having resorted to a lockdown – experts are concerned at why its containment strategy has not been more successful.
Kitty Lee, partner and head of Health and Life Science at the Asia-Pacific arm of consulting firm Oliver Wyman, described the situation as “a bit frightening”.
Lee said residents were “lax” when it came to social distancing, noting that only 40 per cent of employees in the central business district were working from home.
Singapore authorities have since warned employers that those who do not implement telecommuting while being able to do so will face prosecution.
Infectious diseases specialist Leong Hoe Nam said the public needed to be more “aggressive” when it came to social distancing. “There is not enough, currently, to break the epidemic. Rather, the epidemic is breaking us because of the lack of will on the part of the citizens.”
Professor Teo Yik Ying, dean of the National University of Singapore’s Saw Swee Hock School of Public Health told The Straits Times that if Singaporeans refused to “follow simple instructions, then no matter what the government puts in place, we will see an uncontrollable outbreak”.
The greater emphasis on social distancing measures comes amid new research suggesting the virus can spread even before patients show symptoms.
In an article on the United States Centres for Disease Control and Prevention’s website on Wednesday, Singapore researchers including Vernon Lee, director of communicable diseases at the Ministry of Health, detailed how five patients who were not showing symptoms had spread the virus to seven others.
The report concluded that “it might not be enough for only persons with symptoms to limit their contact with others because persons without symptoms might transmit infection”.
In a Caixin Global webinar last Thursday, Lee said Singapore’s reproduction rate of the disease was under one. This meant on average, an infected person in Singapore spread the coronavirus to fewer than one other person. It was 2.35 in Wuhan, China, where the outbreak was first discovered, before the city was locked down.
TO MASK OR NOT?
The rise in local transmissions has also sparked a debate on the merits of wearing face masks.
Previously, Singapore authorities have told people not to because it needed to preserve supplies for health care workers. The advice echoes guidelines by the World Health Organisation.
But the WHO and the United States are both now reviewing those guidelines. Some experts in Hong Kong and Japan argue that widespread mask-wearing cultures have helped them keep the number of infections down.
“There is a very serious question about the wearing of masks, especially in high human traffic places such as the train and so on,” said Professor Lim.
However, he cautioned that wearing masks could also give people a false sense of security, causing them to relax social distancing measures, much as wearing seat belts could lead to more reckless driving.
Infectious diseases expert Leong Hoe Nam said Singapore now faced two challenges: not enough masks for the whole population and the need to get more people to practise social distancing.
Without more action, the health care system could be overwhelmed by the “exponential” growth of the virus, the expert said.
Even amid the gloom, there are reasons for optimism. The home-grown gaming firm Razer has said it will start manufacturing face masks locally within 30 days, while some experts are hopeful the government’s toughening stance on working from home will have an effect.
Still, there is also an awareness that there may be a limit to what can be done, with Lim saying the government was running out of options for even tighter social distancing measures.
Even the minister Wong admitted this week that taking more drastic measures, such as a mooted two-week lockdown, would offer no “magic solution”. Rather, he said, Singapore was prepared to apply a series of “brakes” for the long-haul.
Said Lim: “There are probably just three things left to do: close schools, shut down public transport and order all eating places and malls to shut. I’m not sure what else you can do.”
This article appeared in the South China Morning Post print edition as: Singapore steps up measures to fight ‘second wave’ surge
No comments:
Post a Comment